Having spent a good part of my journalistic career covering crime stories, it’s hard for me to stay away from any crime or medical forensic drama. So when Scarpetta premiered on Amazon Prime Video on March 11, I was immediately drawn in. Partly for the forensic angle, partly because the series is based on Patricia Cornwell’s bestselling novels.
Starring Nicole Kidman as forensic pathologist Kay Scarpetta, the show follows complex investigations that blend medical expertise with criminal cases. But as the story unfolds, it moves beyond traditional forensic themes and into something more unexpected: 3D bioprinted human organs.

How the Amazon Prime show Scarpetta shows 3D bioprinted organs will look like. Image courtesy of Amazon Prime.
A central part of the plot revolves around a fictional biotech company, Thor Labs, which is portrayed as already capable of 3D bioprinting human organs in microgravity, an environment scientists believe could make it easier to build complex biological structures.
In reality, the closest real-world equivalent to the show’s Thor Labs is Redwire, which conducts bioprinting experiments aboard the International Space Station. And while it has already demonstrated early tissue printing in microgravity, it remains far from producing fully transplantable human organs, in pre-clinical trials or beyond.

Live human heart tissue bioprinted with Redwire’s BioFabrication Facility aboard the ISS. The tissue was successfully returned to Earth in April 2024. Image courtesy of Redwire.
The show has taken a real concept, space-based bioprinting, and pushes it a decade or more ahead of where the science stands today. That’s where the line between fiction and reality starts to blur. The question is: how close are we, really?
Nobody is printing a fully transplantable human heart, kidney, or liver yet. But a few groups are clearly closer than the rest, and they fall into three groups: organ-scale scaffolds and bridge tissues, vascularization, and implantable tissues. The most aggressive efforts include United Therapeutics/3D Systems, ARPA-H-backed work at Carnegie Mellon, and research at Stanford, while more clinically focused work is happening at Wake Forest, Poietis, KIT, and in Sydney’s 3D printed skin trials. At the same time, on-orbit bioprinting research continues in places like Tsinghua University in China. Here’s a closer look at some of the groups leading this work:
United Therapeutics + 3D Systems (U.S.)
This is probably one of the most ambitious efforts in the field. United Therapeutics (UT) is developing a 3D printed lung scaffold as part of its ULung program, designed to be populated with human cells. ULung is one of UT’s four pre-clinical and clinical organ and organ alternative platforms designed to address the ongoing shortage of transplantable organs for patients with end-stage organ disease. The company says these structures have already demonstrated gas exchange in animal models and is also working toward printed kidneys and livers. While this is still far from a transplant-ready organ, it remains one of the clearest examples of how far organ-scale bioprinting is being pushed today.

3D bioprinted lung lobe. Image courtesy of United Therapeutics.
ARPA-H PRINT program + Carnegie Mellon and Adam Feinberg (U.S.)
This is the most important U.S. government push. ARPA-H launched its PRINT program to pursue personalized, on-demand organs that would not require immunosuppressive drugs. Among the researchers involved is Adam Feinberg of Carnegie Mellon University, one of the leading experts in 3D bioprinting, who secured support for a 3D bioprinted liver tissue project designed as a temporary alternative for acute liver failure. The goal is to support patients for two to four weeks while their own liver recovers. This is not a permanent replacement, but one of the most realistic short-term solutions to support patients rather than replace the organ entirely.

FRESH 3D bioprinted perfusable liver tissue inside a bioreactor. Image courtesy of Carnegie Mellon.
Stanford’s Mark Skylar-Scott (U.S.)
One of the biggest challenges in bioprinting is vascularization, the ability to create blood vessel networks inside an organ. In 2025, researchers at Stanford University, including bioengineer Mark Skylar-Scott, developed new tools to design and print these vascular structures. This matters because without a working blood supply, larger tissues cannot survive. While this is still not ready for printing a transplant-ready organ, it is working on one of the key problems the field needs to solve for any future printed organ to work.

At the back of the lab, next to a multi-axis bioprinter — a custom machine developed in-house by the Lewis Lab, first pioneered by Jennifer Lewis and her then-postdoc Mark Skylar-Scott. Today, it anchors much of the lab’s effort to print complex, living tissues. Image courtesy of 3DPrint.com.
Wake Forest Institute for Regenerative Medicine and Anthony Atala (U.S.)
Wake Forest stands out for bringing research into real-world use. The institute says it was the first to engineer lab-grown organs that were successfully implanted in humans, and it continues to work across a wide range of tissue and organ research. Not all of this work involves 3D bioprinting; some of its best-known results come from broader tissue engineering, but when it comes to real progress in organ replacement, Wake Forest remains one of the most credible groups in the field, led by regenerative medicine pioneer Anthony Atala.

Young-Joon Seol at the Wake Forest Institute for Regenerative Medicine (WFIRM) demonstrates Bioprinting muscle tissue. Image courtesy of WFIRM.
Poietis (France)
In Europe, Poietis stands out not for claiming full organs, but for working toward implantable tissues. The company says its laser-based bioprinting platform is designed to meet the consistency and quality needed for clinical use, with a clear focus on moving from design to implantation. This means it is developing ways to reliably produce living tissues for real medical use. It makes Poietis a strong example in Europe.

Poietis’ NGB-R bioprinting platform. Image courtesy of Poietis.
KIT + Ute Schepers (Germany)
Work at the Karlsruhe Institute of Technology on a tiny 3D printed baby heart valve shows how the field may reach the clinic sooner through parts of organs rather than whole ones. In this case, researchers used 3D printing to create a biodegradable heart valve scaffold designed to be seeded with the patient’s own cells and grow inside the body. A valve is not a full heart, but it is a more realistic near-term target and still medically important. It’s a good example of how progress in this space is likely to happen, not through fully printed organs overnight, but through smaller, implantable structures.

3D printed baby heart valve. Image courtesy of Uli Deck/dpa/Karlsruhe Institute of Technology.
Tsinghua-led work in China
China is also active in this space, with institutions like Tsinghua University leading research efforts. Public profiles from Tsinghua show active research in cardiac regeneration, on-orbit bioprinting, vascular networks, AI-driven bioprinting, and even papers about on-demand organ manufacturing. This does not mean China has secretly solved printed organs. It shows the country is making progress in several key areas at once, including space-based bioprinting, blood vessel growth, and organoid research.
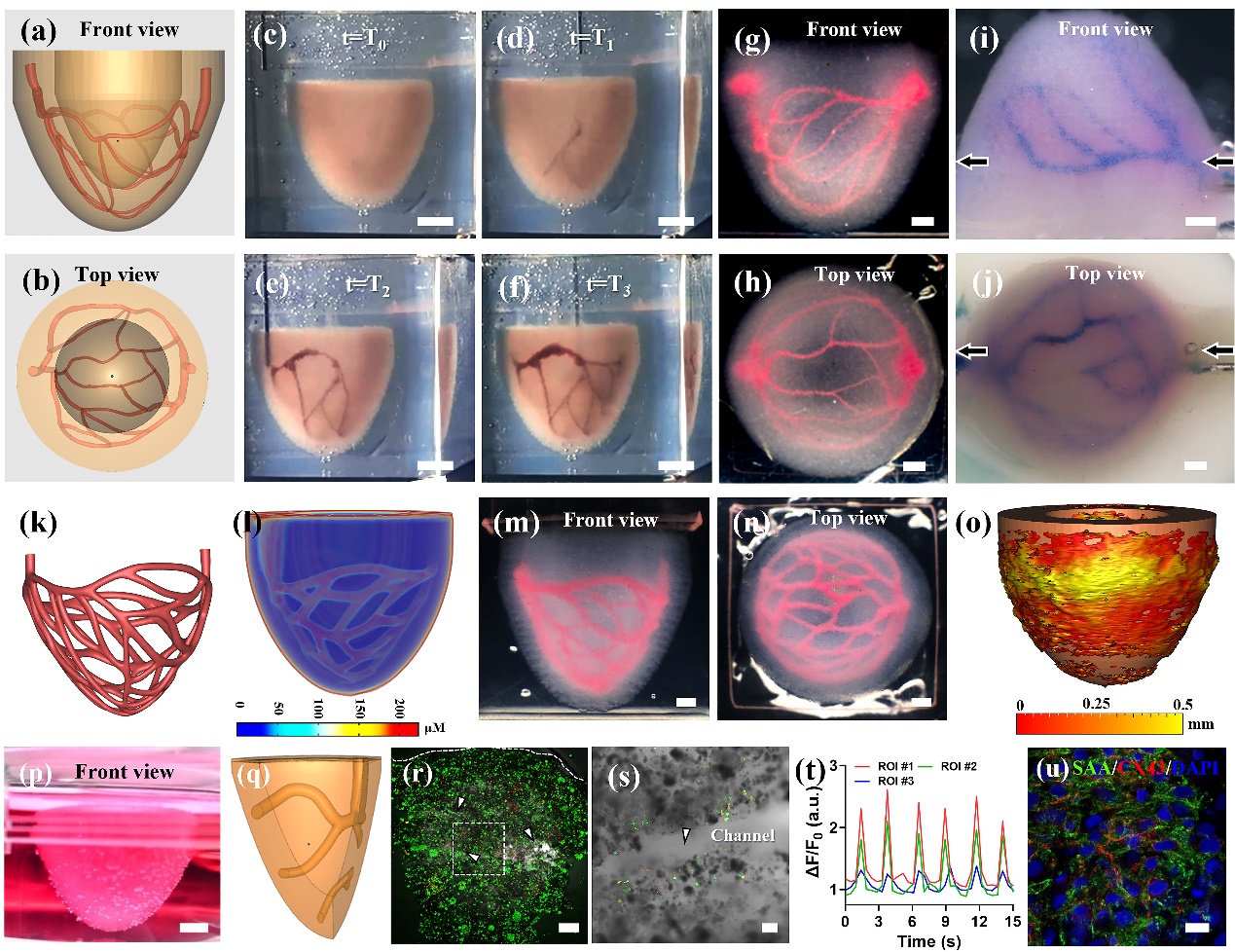
Perfusable ventricle constructs fabricated by SPIRIT. Image courtesy of Tsinghua University.
ANU and the Sydney skin trial
At the Australian National University, bioprinting is being explored as a path toward future organs, with current work focused on printing living cells, tissue-like structures, and organoids for disease modeling. A clearer example is Sydney’s world-first 3D printed skin trial using a patient’s own cells. Skin is not a kidney, but it is still a living, printed tissue used in a real medical setting, showing where the field is starting to have a real impact.

Dr Jo Maitz with NSW Health Minister Ryan Park and Strathfield MP Jason Yat-Sen Li during a visit to Concord Burns Unit. Image courtesy of Concord Burns Unit.
It will likely be some time before we see the kind of lab-grown, microgravity-grown organs ready for clinical use, as seen in Scarpetta. But the idea is not entirely out of reach. If anything, it’s a reminder of where the technology is heading, and a good way to put the spotlight on a field that is moving forward.

Nicole Kidman as forensic pathologist Kay Scarpetta in Scarpetta. Image courtesy of Amazon Prime.
